Expert Voice: Does leadership style in the management of end-of-life care impact patient choice?
Jo Laidlaw presented this topic at the National Hospice UK Conference in Liverpool

Does the leadership style applied in the management of end-of-life care services impact patient choice? A systematised review.
By Jo Laidlaw, Hospice@Home Team Leader, Moya Cole Hospice
Introduction and Background:
The dissertation was completed in partial fulfilment of the requirements for the MSc Leadership and Management Clinical Leadership in Action Program.
The researcher identified that research in palliative care and leadership styles is limited. The number of patients being supported in the community with life-limiting illness is increasing (1). People are living longer with multiple long-term conditions (2). Home is chosen as PPD but only 25% of patients achieve this (3). The reason for this is thought to be due to accessibility of services (4).It has been identified that development, change and review of services is required to improve patient outcome and enable choice at end of life (5). The leadership role is essential in the delivery and quality of healthcare services to improve patient outcome (6).
Aims and Objectives:
- To undertake a systematised review of the available literature related to leadership styles in EOLC and their impact upon choice at EOL.
- To apply critical appraisal tools to evaluate the methodological quality of the included studies.
- To evaluate the application of leadership styles and their effectiveness in EOLC settings.
- To critically review the impact of leadership styles in care delivery and patient choice in EOLC.
- To make recommendations for practice.
Findings:
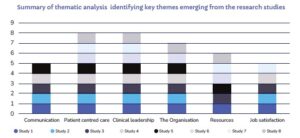
Eight studies were included in the systematised review – four qualitative studies and four cross-sectional studies. Application of thematic analysis identified six emerging themes relevant to the review question – Communication, patient centred care, clinical leadership, the organisation, resources and job satisfaction.
Results:
Effective communication between team leaders and staff had a positive impact on patient outcome.
Patient satisfaction should be considered when a leader is adopting a leadership style.
Leadership was identified as essential in healthcare for effective team management and to achieve organisational aims. It was found that it is not a requirement for leaders to be managers, nursing staff can adopt a leadership role and they may be best placed for this due to their experience and knowledge.
Transformational leadership style was found to be the most favourable leadership style in healthcare organisations. It was found that transformational leaders influence staff and the team in a positive way, they recognise staff achievements, communicate effectively, and encourage teamwork, resulting in job satisfaction leading to effective patient care, identifying that if patients are receiving quality care they are more likely to choose that care.
It has been found that with the current evidence that the leadership style alone does not impact patient choice it does influence the team that is providing patient care. It was found that an effective leader will lead a team, with communication, increased morale, positivity, collaboration and job satisfaction, which then will enable the team to deliver quality care leading to impact on patient choice.
Authentic leadership has a positive effect in the delivery of palliative care. Transactional leadership is not a preferred style of leadership in healthcare settings.
Laissez faire identified as a negative leadership style with a negative impact on organisations.
A leader may need to adopt different leadership styles dependent on the situation.
Recommendations for practice:
Develop and sustain educational programmes accessible to all staff to enable development and awareness of leadership and leadership styles in line with the organisational aims, values, mission and vision.
Training and awareness in the application of specific leadership styles according to patient group and the organisation.
This systematised review to be available to all staff within the organisation for information and knowledge.
For leadership and leadership styles impact on patient care and outcomes to be on team meetings agenda for all staff to receive the same information.
Current leaders within the organisation to share their work and experience in the leadership role.
For staff to take on elements of leadership roles to gain experience and to shadow leaders in their role as appropriate.
For leaders to set times to be available on an informal level for staff to meet with to gain understanding of leaders and their role also for leaders to communicate with staff.
Ensure patient feedback questionnaires reflect on leadership and leadership styles to gain an understanding from the patient’s perspective.
References
- Mitchell S, Loew J, Millington-Sanders C & Dale J. Providing end-of-life care in general practice: findings of a national GP questionnaire survey.British Journal of General Practice.(2016); 66(650), 647-653.
- Anon. The Parliamentary Office of Science and Technology – Bridging research and policy. (2022); [online] Available at: https://post.parliament.uk/.
- Higginson I.J, Daveson B.A, Morrison R S, Yi D, Meier D, Smith M, Ryan K, McQuillan R, Johnston B.M & Normand C. Social and clinical determinants of preferences and their achievement at the end of life: prospective cohort study of older adults receiving palliative care in three countries. BMC geriatrics. (2017); 17,1-14.
- Mistry B, Bainbridge D, Bryant D, Toyofuku S.T, & Seow H. (2015). What matters most for end-of-life care? Perspectives from community-based palliative care providers and administrators. BMJ open. (2015); 5(6), e007492.
- GREATER MANCHESTER COMMITMENTS TO PALLIATIVE CARE INDIVIDUALS APPROACHING OR WITHIN THE LAST YEAR OF LIFE – What an individual with Palliative and End of Life Care needs should expect across Greater Manchester. Available at: https://gmintegratedcare.org.uk/wp-content/uploads/2022/06/07a-greater-manchester-approach-for-palliative-and-end-of-life-care-final-gm-palliative-and-end-of-life-care-commitments-hcb-31052019-final-v10.pdf. (2022).
- NHS England. NHS England» Ambitions for Palliative and End of Life Care: a National Framework for Local Action 2021-2026. [online] www.england.nhs.uk. Available at: https://www.england.nhs.uk/publication/ambitions-for-palliative-and-end-of-life-care-a-national-framework-for-local-action-2021-2026/.(2021)
